
Fulminant Lymfocytic myocarditis Treated with ECMELLA and Immunosuppression
19-year-old woman with past medical history of atopic eczema presented to a regional hospital after 2 days of gastrointestinal symptoms (diarrhoea and vomiting) with a third-degree atrioventricular block, left ventricular (LV) systolic dysfunction (LV ejection fraction 40%).
Laboratory findings (on admission)
- high sensitivity troponin T - 13 850 ng/L (normal range, 0-14 ng/L)
- N terminal pro brain natriuretic peptide - 19 686 ng/L (normal range, 10-155 ng/L)
The patient’s condition quickly progressed to a cardiogenic shock requiring inotropes, temporary transvenous pacing (complete AV block), and tracheal intubation.
Coronary angiography was performed and showed patent arteries. Within the next day, her status further deteriorated with development of severe biventricular dysfunction and multiple organ failure.
Urgent insertion of transfemoral veno-arterial extracorporeal membrane oxygenation (VA ECMO) was indicated as her global LV ejection fraction dropped to <10%.
Video 1 Severely impaired left ventricular dysfunction documented on TTE

Right ventricular endomyocardial biopsy (EMB) revealed diffuse lymphocytic myocarditis, resembling severe cellular allograft rejection, with interstitial oedema and mild myocyte necrosis.
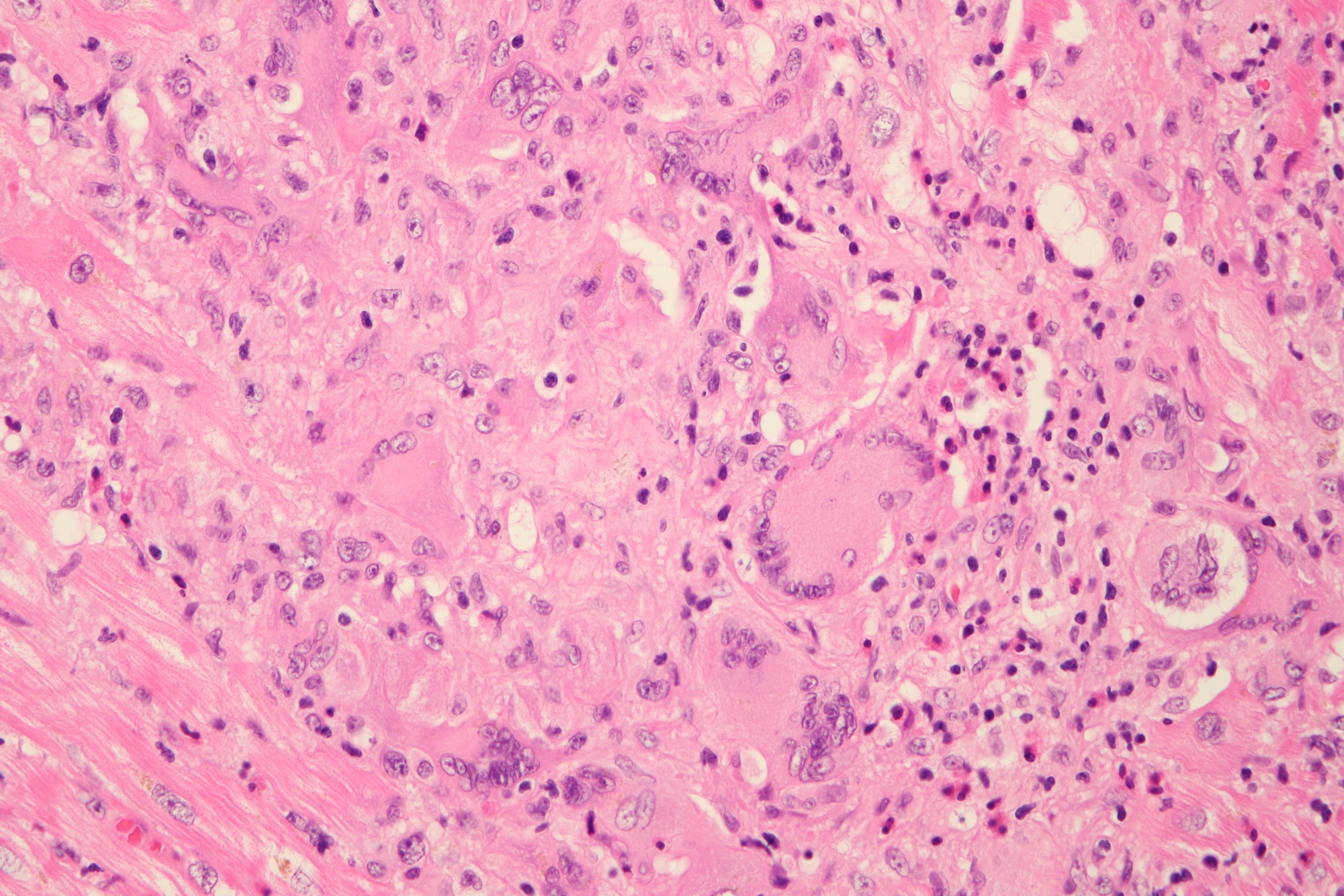
Figure 1 Right ventricular endomyocardial biopsy (EMB)

Lymphocytic myocarditis. Haematoxylin–eosin, original magnification (i) ×200 and (2) ×400. (A) Normal myocardial fibres. (B) Myocardial necrosis with interstitial inflammatory oedema and infiltrate, mostly lymphocytic.
PCR for detection of viral pathogens in the EMB specimen was negative. In addition to conventional histology, multichannel flow cytometry was used on myocardial sample to reveal the nature of myocardial inflammation. Evidence of cytotoxic CD8 T-cell predominance was found, accompanied by activation status of the entire T lymphoid compartment.
Figure 2 Composition and activation status of intramyocardial leucocyte compartments. Flow cytometry from endomyocardial biopsy (EMB) tissue.

(A) CD4/CD8 balance in myocarditis EMB vs. autopsy control (gated on CD3+CD11bnegCD19neg viable cells), showing a reversed CD4/CD8 ratio in myocarditis. (B, C) Activation status of CD4 T cells and CD8 T cells, respectively, based on CCR7/CXCR3 status, showing in both subsets a shift toward a predominant CCR7neg effector status in myocarditis EMB. (D) Functional subsets of heart infiltrating macrophage/monocytes (gated on CD11b+CD19neg CD3 should not be in normal case (not in superscript) CD66bneg viable cells), showing a predominant pro-inflammatory phenotype CD14int/+CD16neg in myocarditis EMB.
Because of clear evidence of immune-mediated origin, immunosuppression with 1 g/day (in 3 days) of methylprednisolone (Solu-Medrol, Pfizer) and intravenous immunoglobulin G (0.5 g/kg of body weight; Privigen, Behring) was instituted.
Two days after ECMO implantation, the patient developed episodes of refractory sustained ventricular tachycardia requiring repeated cardioversions, accompanied by worsening of pulmonary gas exchange.
Figure 3 ECG with ventricular tachycardia (224/min)

In order to achieve better venting of stagnating LV cavity, Impella 2.5 (Abiomed) pump was introduced via transfemoral access. With such ‘ECMELLA’ (ECMO + Impella) configuration, ventricular tachycardia ceased and prompt stabilization was achieved.
Day 7 - Impella 2.5 was exchanged for an Impella 5.0 device introduced via a graft sewn on a right subclavian artery, a device that has longer durability and full-flow support capability.
Figure 4 Chest radiogram shows venous cannula of extracorporeal membrane oxygenation (ECMO) circuit (black arrow), Impella 5.0 inflow segment in the left ventricle (red arrow), and outflow segment in aorta (yellow arrow).

Immunosuppression was continued with oral prednisone 1 mg/kg/day.
Day 10 - echocardiogram showed marked improvement of systolic function of ventricles (left ventricular ejection fraction > 60%).
Video 2 TTE with normalized LV ejection fraction (Impella 5.0 inserted into the LV).

Day 11 - ECMO was discontinued.
Day 13 - Impella was explanted and the patient remained hemodynamically stable.
Further recovery was uneventful, and the patient was discharged after 44 days.
At the discharge:
- patient had normal cardiac function by echocardiography and cardiac magnetic resonance imaging, without evidence of late gadolinium enhancement (consistent with lack of scar development)
- normal BNP and troponin levels
- incomplete right bundle branch block on ECG
Figure 5 ECG at the discharge with incomplete right bundle branch block.

Clinical context and take home messages
Fulminant myocarditis (FM) is a rare and severe form of myocarditis that presents with sudden onset of acute heart failure, cardiogenic shock, and/or life-threatening arrhythmias.
FM may be of viral, bacterial, toxic, or autoimmune origin. The damage of the myocardium may result from direct cardiomyocyte insult or from indirect injury by immune-mediated cytotoxicity or tissue oedema.
The diagnosis and treatment of FM are still a clinical challenge owing to variability of clinical presentation and limited use of myocardial biopsy.
The management often requires intensive care, inotropic and mechanical circulatory support (MCS),
and sometimes immunosuppressive therapy. Early institution of MCS and early myocardial biopsy to ascertain prognosis and to guide immunosuppression is critical to successful management of FM.
ECMO increases the chances of recovery/long-term survival for patients with the most dramatic presentations. However, ECMO is often not enough to achieve decompression of stagnating left ventricle, which may lead to:
- lung oedema
- LV intracavitary thrombus
- impaired myocardial tissue drainage
Methods for unloading of ECMO-supported left ventricle include:
- intraaortic balloon pump
- Impella
- direct surgical LV venting - depends on the individual clinical settings, risk of the intervention, local. experience, and the time expected for recovery.
Impella is a catheter-based miniaturized ventricular assist device. It is placed in the left ventricle across the aortic valve. The device pumps blood from the left ventricle into the ascending aorta and helps to maintain a systemic circulation at a rate between 2.5 and 5.0 L/min. This results in almost immediate and sustained unloading of the left ventricle, while increasing overall systemic cardiac output. The Impella 2.5 model is inserted via a retrograde femoral arterial approach, similar to the technique used for placement of an IABP. The larger sized Impella 5.0 model requires an arteriotomy for placement.
Immunosuppressive therapy in lymphocytic FM is still not yet fully defined due to lack of randomized human studies, but offers new therapeutic ability for FM management. It may be considered if acute viral infection in the biopsy is ruled out and if there is a high likelihood of autoimmune aetiology, especially in patients with pre-existing autoimmune disease
References
- Jurcova I, Rocek J, Bracamonte-Baran W, et al. Complete recovery of fulminant cytotoxic CD8 T-cell-mediated myocarditis after ECMELLA unloading and immunosuppression. ESC Heart Fail. 2020;7(4):1976-1981. doi:10.1002/ehf2.12697
- Glazier JJ, Kaki A. The Impella Device: Historical Background, Clinical Applications and Future Directions. Int J Angiol. 2019 Jun;28(2):118-123. doi: 10.1055/s-0038-1676369. Epub 2018 Dec 20. PMID: 31384109; PMCID: PMC6679960.
Authors: Ivana Jurcova, Jan Rocek, William Bracamonte-Baran, Michael Zelizko, Ivan Netuka, Jana Maluskova, Josef Kautzner, Daniela Cihakova, Vojtech Melenovsky, Jiri Maly
You Might Also Like
Cardiogenic shock due to Giant Cell Myocarditis
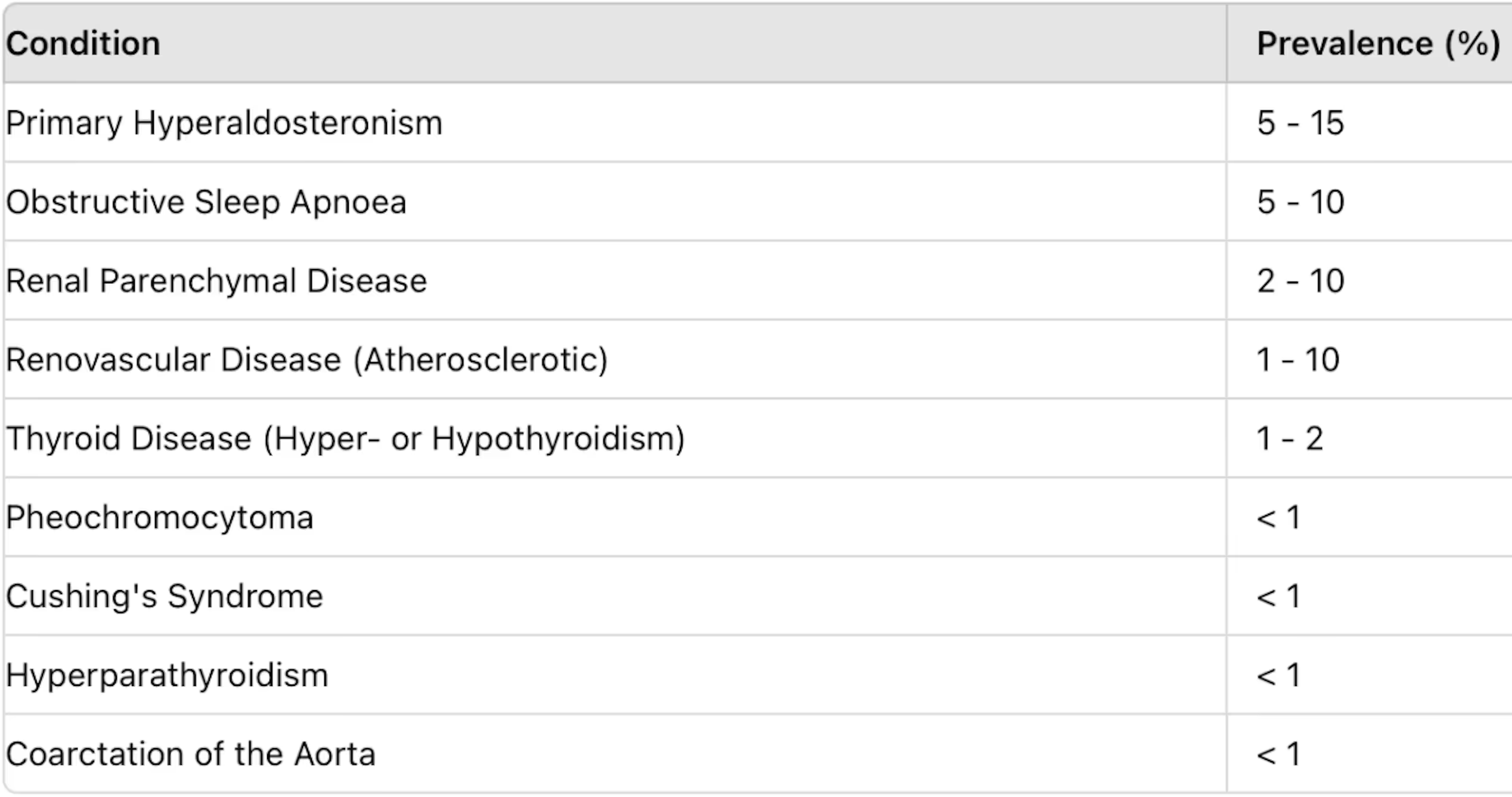
Secondary hypertension

.jpg)


